What is a leg ulcer ?
Located on the lower third of the leg (under the knee), leg ulcers are chronic wounds that have not healed after 6 weeks. The wounds may be caused by a knock, by scratching, or even appear on their own.
Leg ulcers take different forms.
- Venous leg ulcers (70% of cases): related to poor venous circulation. The wound is superficial in most cases, with inflamed, uneven edges. It is painful and mainly located around the ankle.
- Arterial leg ulcers (10% of cases): related to poor arterial circulation. They start out as a small cut with uneven edges on the leg or foot/toes. Gradually becoming deeper, the wound can even go on to reveal the tendons or the bones, as it progressively necrotises (can turn black). The wound is very painful.
- Mixed leg ulcers: related to poor arterial and venous circulation. Signs of a venous ulcer and an arterial ulcer are present at the same time.
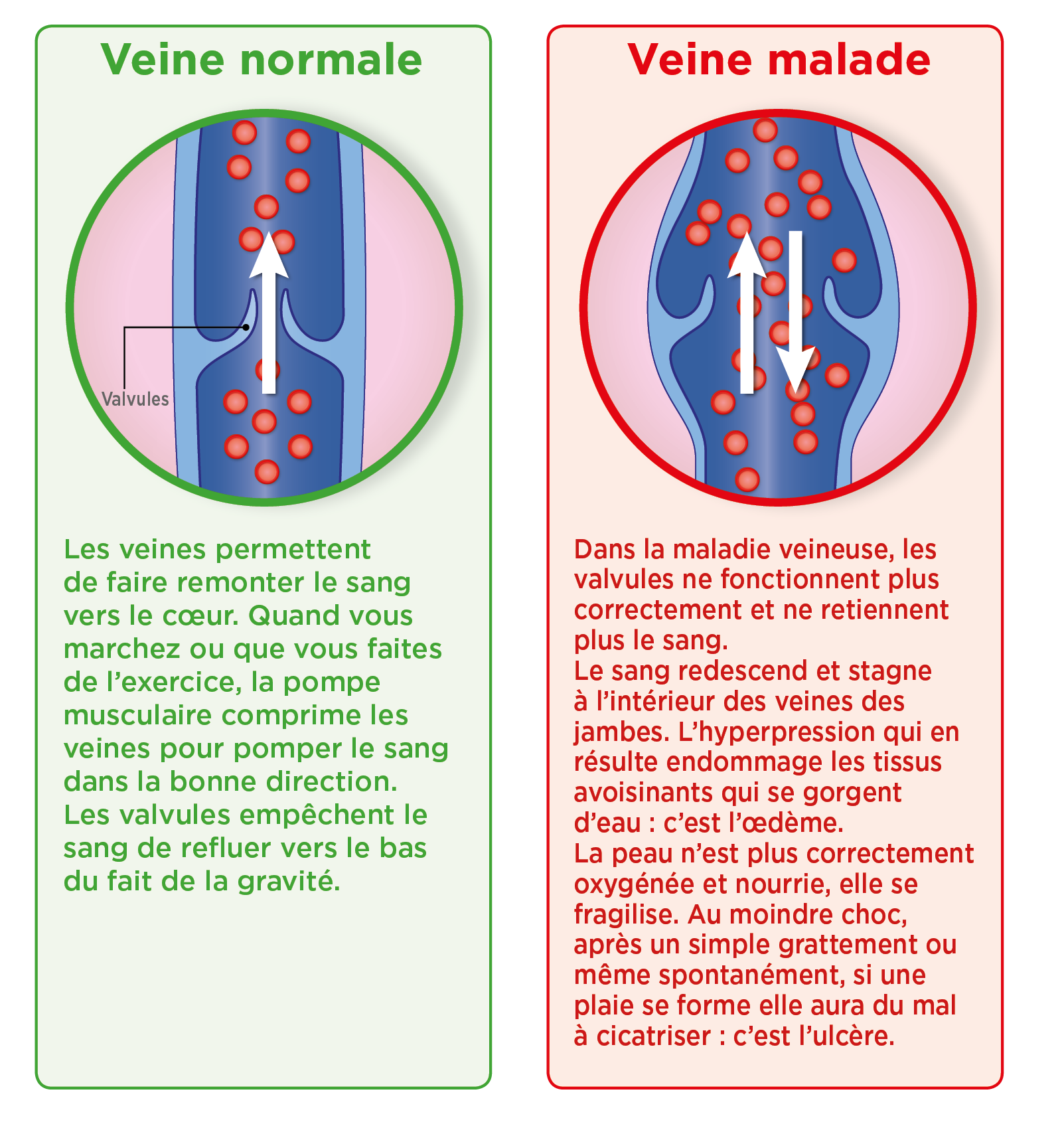
How does a venous ulcer form?
A venous leg ulcer is the result of chronic venous insufficiency which prevents the blood flowing normally in the veins of the leg. Unable to travel along its usual path, the blood stagnates in the leg veins, and goes on to damage the tissue and break the skin.
This is why treatment should come with an in-depth diagnosis, to identify the cause of the venous failure.
Various factors or bad habits can also encourage leg ulcers:
- History of varicose veins or deep vein thrombosis
- Lack of physical exercise
- Arterial hypertension/diabetes
- Being overweight/obesity
- Smoking/alcohol abuse
How is a venous leg ulcer treated?
There are no small ulcers. As soon as you notice a wound or if you have any doubts, contact your doctor as soon as possible. The sooner the ulcer is treated the faster it will heal.
Venous leg ulcers or predominantly venous leg ulcers must be treated by a doctor. Treatment generally begins with careful wound cleansing with soap and water or saline solution, and does not routinely need disinfecting (using an antiseptic may imbalance the skin’s flora and slow healing, or even cause an allergy). This is followed by the application of a wound dressing.
Finally, to help improve venous return and aid healing, compression bandages should be applied and worn continually, followed by lifelong use of compression stockings to prevent recurrence. The good news is that with the use of effective compression therapy,, venous leg ulcer recurrence can be avoided by up to 90%; in contrast, without it, the recurrence rate can reach 97%*.
Finally, a dressing can help treat the wound locally.
Your doctor can prescribe you a dressing to reduce the healing time, based on the available clinical evidence.
In the event of a mixed leg ulcer (both venous and arterial), compression can be indicated but it will be looser than for a venous ulcer. It will depend on the degree of associated arteriopathy.
Compression is not indicated in arterial ulcers.
Avoiding relapse
Taking care of your health and physical condition is the best way of preventing a leg ulcer from recurring. To do that you must ensure:
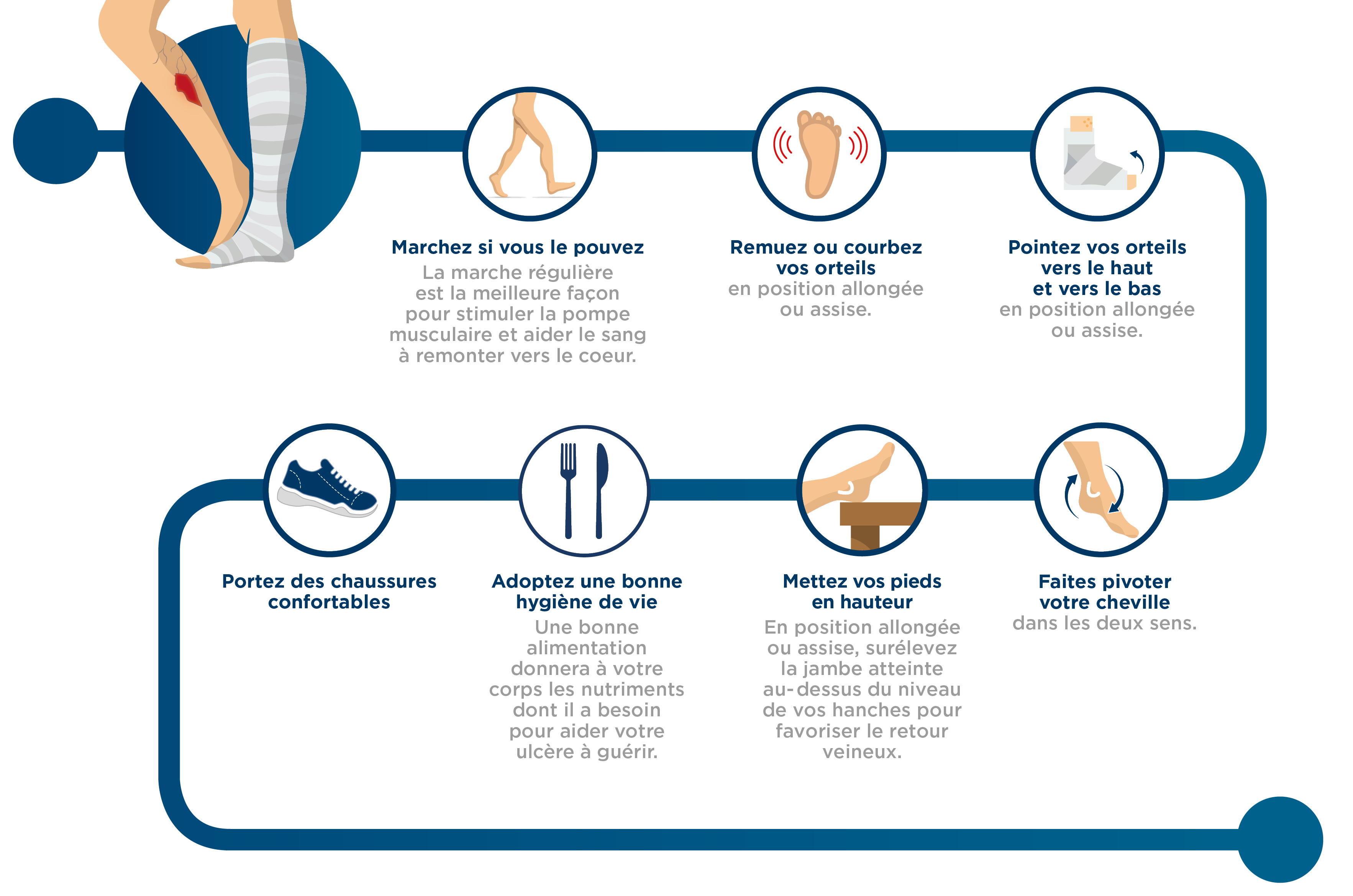
And also:
- Avoid crossing the legs when sitting down
- Avoid hot baths
- Wear your compression stockings
- Wear comfortable, non-slip shoes
- Regularly moisturise your skin
- Adopt a healthy diet (fibres, proteins, vitamins etc.) and a healthy lifestyle (drink plenty of water, stop smoking)
- Prevent weight gain.